Human trafficking is an illegal trade of exploiting people, often those who are more vulnerable. It is defined as using force, fraud or coercion to compel a person into any form of work, whether sex or other labor. Survivors often need many services, but insufficient funding worries some organizations.
State law imposes mandatory fines on people who commit human trafficking and related sexual exploitation crimes, such as commercial sexual abuse of a minor. Fines make those who exploit other people responsible for contributing financially to local efforts to address these crimes and support survivors.
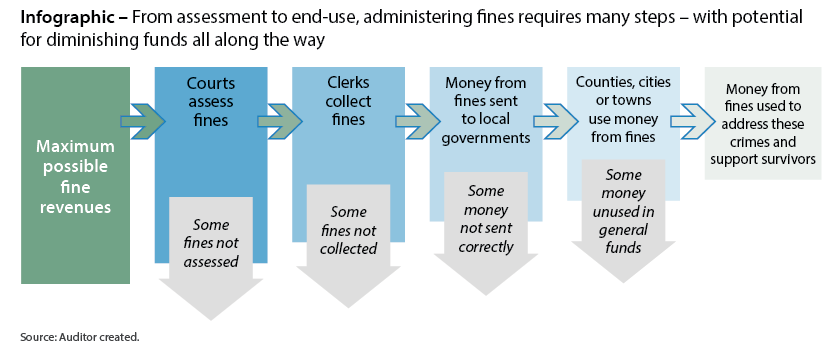
Human trafficking is a serious issue -- criminal activities that are difficult to detect and combat. In this performance audit, we reviewed the assessment, collection and use of court fines associated with human trafficking and sexual exploitation crimes, which are intended to fund efforts to prevent these crimes and support survivors.
Read a 3-page summary of the report.